Insulin resistance often develops quietly around us and is an early sign of diabetes.Today, let’s talk about it.
How Insulin Normally Works
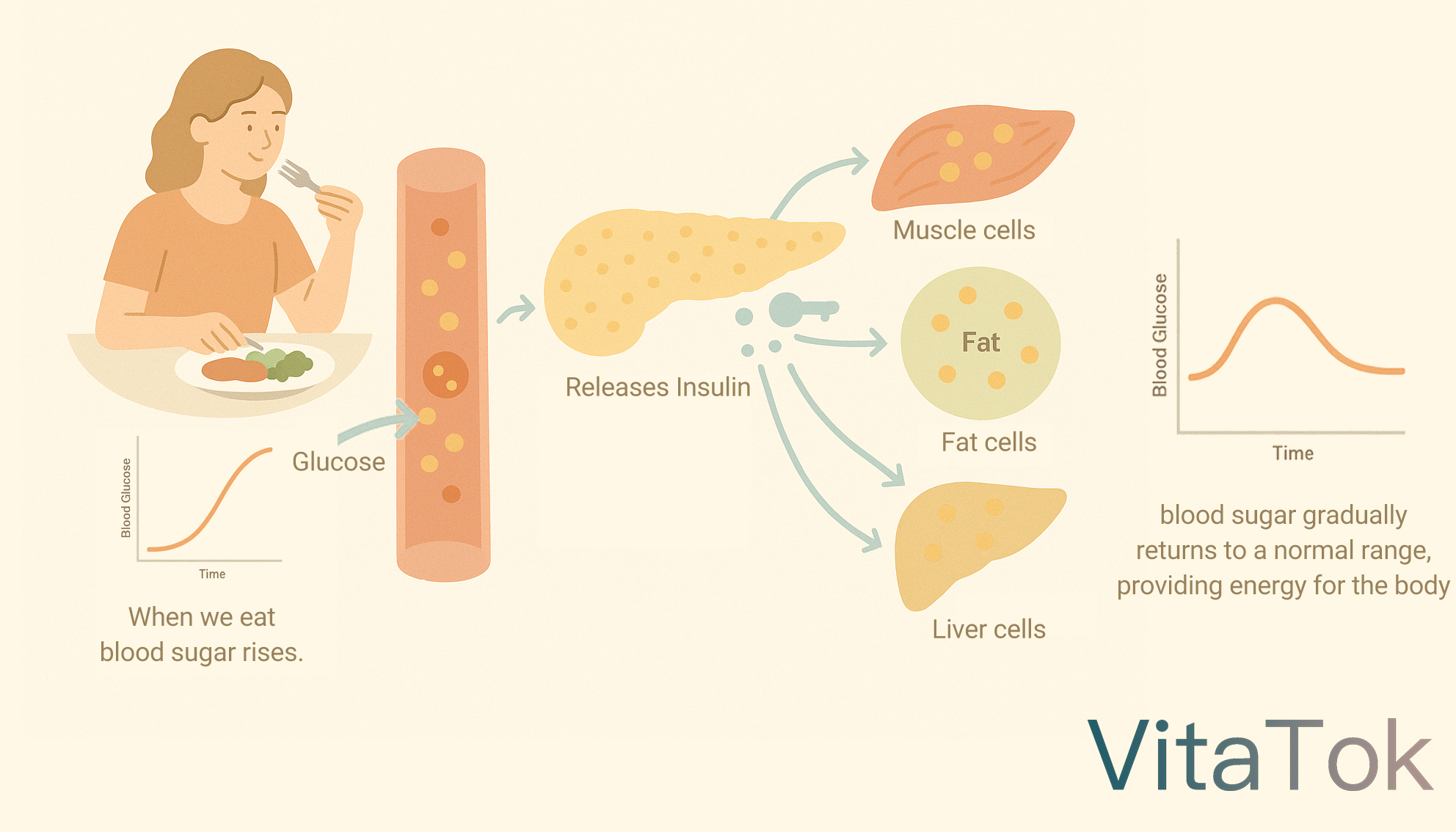

When we eat, blood sugar rises. In response, the pancreas releases insulin. Insulin acts like a “key” that opens the doors of muscle, fat, and liver cells, allowing glucose to enter, where it is converted into energy or stored as glycogen or fat.
As a result, blood sugar gradually returns to a normal range, providing energy for the body without causing excessive blood sugar levels.
When Insulin “Fails” — Insulin Resistance
Insulin resistance occurs when cells become less responsive to insulin. In other words, even if insulin is present in the blood, the cells do not respond effectively, making it difficult for glucose to enter the cells.
To maintain blood sugar levels, the pancreas produces more insulin. This can keep blood sugar normal in the short term. However, over time, the pancreas becomes overworked, its insulin secretion declines, blood sugar gradually rises, and type 2 diabetes may develop.
Common Mechanisms and Causes of Insulin Resistance
- Obesity, especially abdominal fat: Excess fat releases inflammatory factors and fatty acids that interfere with insulin sensitivity in muscle, liver, and fat cells.
- High-fat or high-sugar diet: Chronic excessive energy intake increases fat accumulation and liver fat, reducing insulin effectiveness.
- Lack of exercise: Insufficient physical activity reduces the muscles’ ability to use glucose, lowering insulin efficiency.
- Chronic low-grade inflammation: Persistent inflammation disrupts insulin signaling pathways, making cells resistant to insulin.
- Genetic factors: Some people are naturally less sensitive to insulin and more prone to insulin resistance.
In insulin resistance, glucose remains in the bloodstream, forcing the pancreas to secrete more insulin continuously, resulting in hyperinsulinemia. If left unaddressed, this may lead to metabolic syndrome, including high blood sugar, high blood pressure, and high blood lipids.
💡 Summary: Insulin resistance is not a lack of insulin, but a reduced cellular response to insulin. It makes blood sugar control more difficult and increases the risk of diabetes and cardiovascular disease.
Symptoms of Insulin Resistance
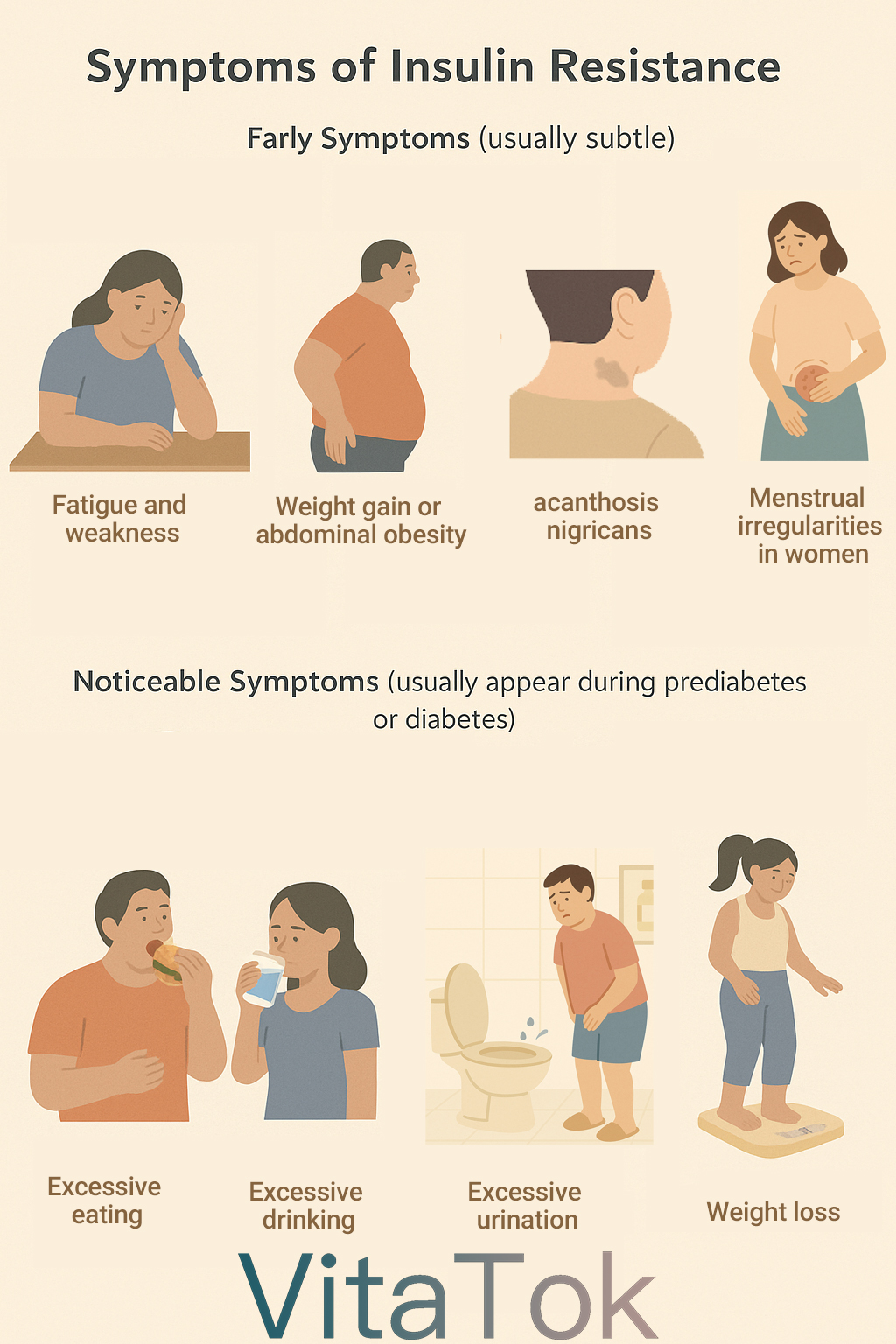

Early Symptoms (usually subtle)
- Fatigue and weakness: Glucose cannot enter cells, leading to low energy and difficulty concentrating.
- Weight gain or abdominal obesity: Waistline gradually increases, visceral fat accumulates.
- Skin changes: Dark, rough patches on the neck, armpits, joints, etc. (acanthosis nigricans).
- Menstrual irregularities in women: Such as cycle disturbances, sometimes associated with polycystic ovary syndrome (PCOS).
Noticeable Symptoms (usually appear during prediabetes or diabetes)
Typical “Three Excesses and One Loss” signs:
- Excessive eating: Always feeling hungry
- Excessive drinking: Persistent thirst, drinking a lot of water
- Excessive urination: High blood sugar causes frequent urination
- Weight loss: Despite increased appetite, body weight decreases
Blood sugar abnormalities: Elevated fasting or postprandial blood sugar, with slow decline after meals.
Who Is at Higher Risk?
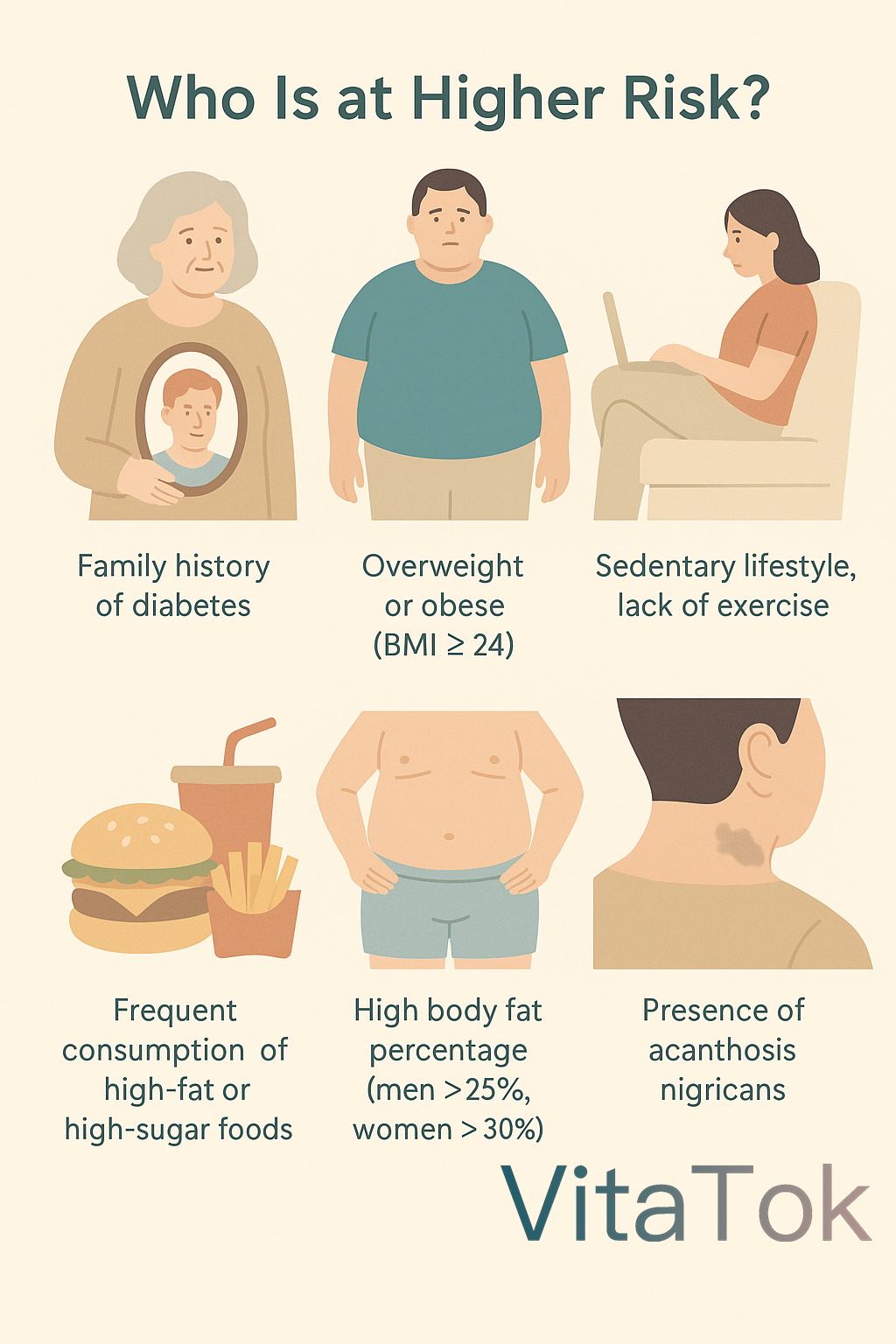

Pay extra attention if you meet any of the following conditions:
- Family history of diabetes
- Overweight or obese (BMI ≥ 24)
- Sedentary lifestyle, lack of exercise
- Frequent consumption of high-fat or high-sugar foods
- High body fat percentage (men >25%, women >30%)
- Presence of acanthosis nigricans (dark, rough patches on the neck, armpits, elbows)
How to Assess Insulin Resistance
Fasting blood glucose alone sometimes fails to reveal the problem. Doctors often use the Homeostatic Model Assessment of Insulin Resistance (HOMA-IR):
- ≤1.4 → Normal
- 1.5–1.9 → Mild resistance
- ≥2.0 → Severe resistance
Formula:
HOMA-IR = (Fasting Glucose × Fasting Insulin) / 405
The Role of CGM in Detecting Insulin Resistance
In the early stage of insulin resistance, single fasting or post-meal blood glucose readings often remain “normal” and may go unnoticed. At this stage, Continuous Glucose Monitoring (CGM) can play an important role.
CGM can record blood glucose levels in real time for 24 hours, helping to observe:
- Whether postprandial blood glucose is too high or declines too slowly
- Whether mild blood glucose fluctuations occur at night or during fasting
- How daily diet and exercise affect blood glucose
These dynamic data can reveal potential insulin resistance earlier, providing valuable reference for doctors and individuals, allowing interventions before diabetes develops.






