1. What is Hypoglycemia?
Hypoglycemia occurs when blood glucose falls below 70 mg/dL.
Hypoglycemia can be classified as:
- Mild (can be self-managed)
- Severe (requires assistance from others or urgent medical care)
Frequent or prolonged hypoglycemia may also affect cardiovascular health and cognitive function.
2. Symptoms of Hypoglycemia
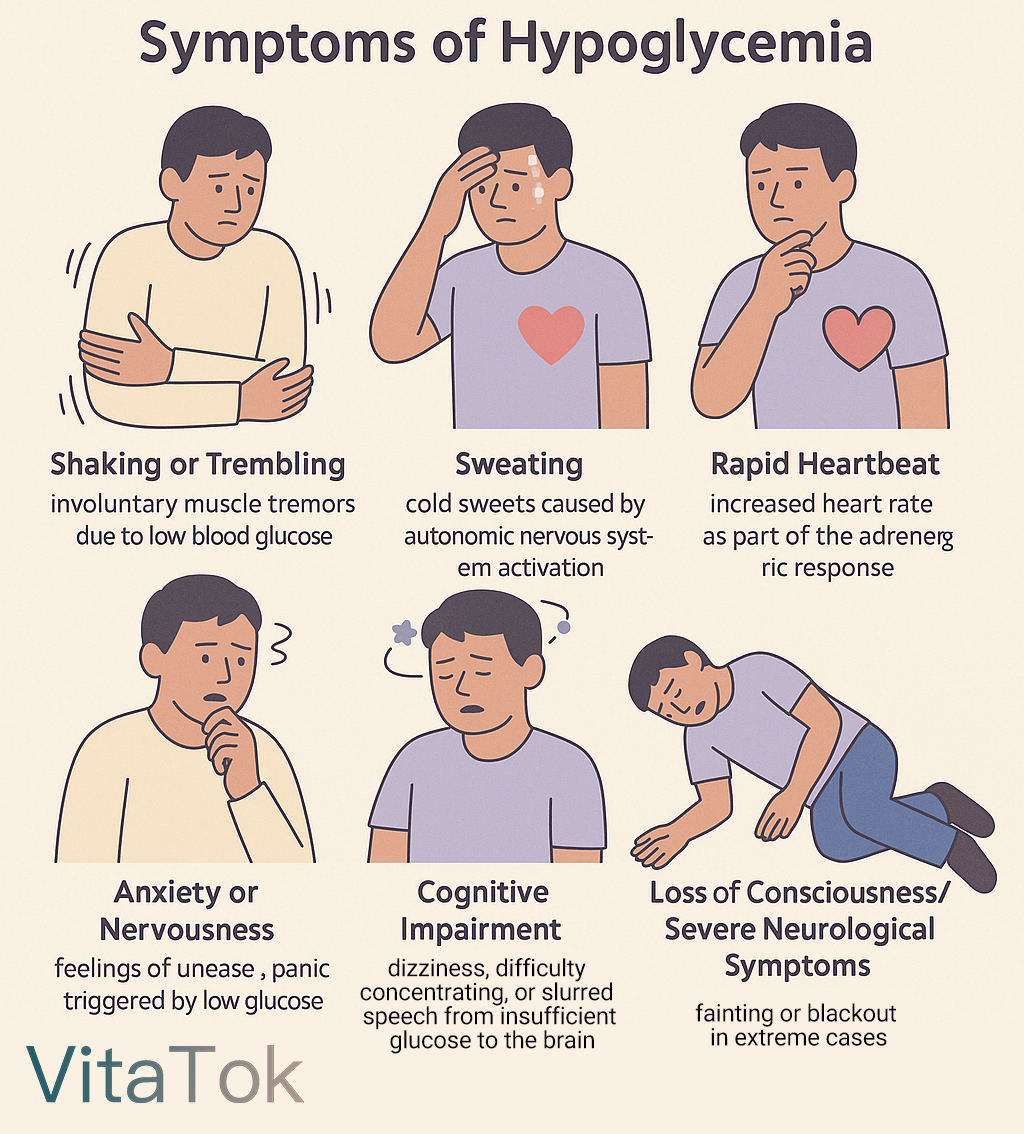

During mild hypoglycemia, autonomic nervous system responses usually appear first:
- Trembling or shaking
- Cold sweats
- Rapid heartbeat
- Anxiety or nervousness
If blood glucose continues to drop, neuroglycopenic symptoms may develop due to insufficient glucose supply to the central nervous system:
- Dizziness
- Blurred vision
- Difficulty concentrating
- Slurred speech
- Loss of consciousness
Additional risks:
- Increased risk of falls, traffic accidents, and other injuries
- Long-term recurrent hypoglycemia may impair cognitive function
- In patients with diabetes, it may interfere with glucose management and increase complication risks
👉 Therefore, when these symptoms occur suddenly, blood glucose should be measured promptly to confirm hypoglycemia.
3. Causes of Hypoglycemia


-
Reactive Hypoglycemia
Occurs about 2–5 hours after meals. Rapid post-meal glucose rise may trigger excessive insulin secretion, causing blood glucose to drop too low. -
Exercise-Induced Hypoglycemia
Physical activity increases insulin sensitivity, causing muscles to absorb glucose quickly. High-intensity or prolonged exercise without timely carbohydrate intake can easily lead to hypoglycemia. -
Excessive Alcohol Consumption, Especially on an Empty Stomach
Alcohol inhibits gluconeogenesis, preventing the body from restoring blood glucose to normal when it is low, which can trigger hypoglycemia. -
Medication Effects
Improper dosage or timing of glucose-lowering drugs or insulin, or a mismatch with food digestion rate, can result in excessive postprandial blood glucose drop. -
Skipping Meals or Not Eating
Long gaps between meals or insufficient carbohydrate intake can cause blood glucose to drop too low, especially in people taking insulin or glucose-lowering medications.
4. How to Manage Hypoglycemia
Mild Hypoglycemia (Self-Managable)
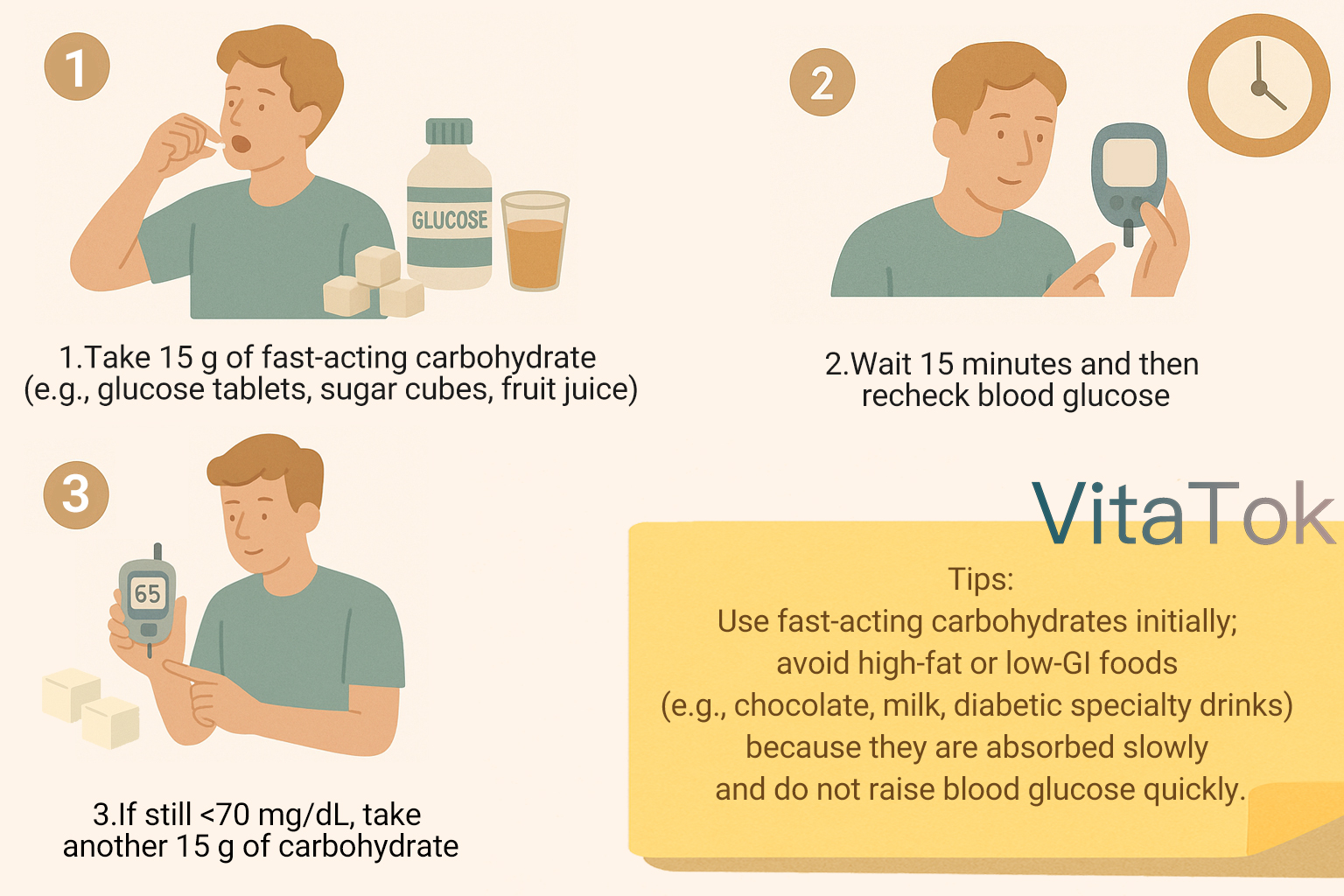

Follow the 15–15 Rule:
- Take 15 g of fast-acting carbohydrate (e.g., glucose tablets, sugar cubes, fruit juice)
- Wait 15 minutes and then recheck blood glucose
- If still <70 mg/dL, take another 15 g of carbohydrate
Make sure blood glucose rises to ≥70 mg/dL before stopping treatment.
Severe Hypoglycemia (Unable to Self-Manage / Unconscious)


- Administer glucagon to help restore blood glucose.
- If injection is unavailable, place honey or syrup inside the patient’s oral cavity for absorption.
- If symptoms do not improve, seek emergency medical care immediately.
Note: Use fast-acting carbohydrates initially; avoid high-fat or low-GI foods (e.g., chocolate, milk, diabetic specialty drinks) because they are absorbed slowly and do not raise blood glucose quickly.
5. How to Prevent Hypoglycemia
Dietary Habits
- Eat regular, balanced meals; do not skip or delay meals.
- Choose low-GI carbohydrates or complex carbs, combined with protein and healthy fats to reduce glucose fluctuations.
- Carry candy, biscuits, or sweetened drinks for emergencies when outside.
Exercise and Activity
- Check blood glucose before exercise; if low, consume carbohydrates first.
- During high-intensity or prolonged exercise, take carbohydrates during and after activity.
- Pay special attention to post-exercise nutrition to prevent nighttime or next-day hypoglycemia.
Medication and Insulin Management
- Understand the timing and action profile of personal medications or insulin.
- Coordinate medication with meals and activity; do not stop medication on your own.
- If hypoglycemia occurs three times or more per week, consult the healthcare team to adjust treatment.
Nighttime Hypoglycemia Prevention
- Test blood glucose before bedtime; if <110 mg/dL, take a small carbohydrate snack (e.g., milk, whole-grain crackers).
- If nighttime hypoglycemia occurs frequently, consider using a Continuous Glucose Monitor (CGM) to track overnight glucose trends.
Monitoring and Review
- Regularly monitor blood glucose (fingerstick tests or CGM) to understand fluctuations throughout the day.
- After hypoglycemia, review causes (meal timing, exercise, medication) and record them to prevent recurrence.
- If hypoglycemia occurs at consistent times, discuss solutions with a physician or dietitian.
6. Advantages of CGM in Preventing Hypoglycemia
- Real-Time Monitoring: Tracks glucose trends continuously, reducing the chance of missed hypoglycemia.
- Timely Alerts: Automatically notifies when glucose is too low or dropping rapidly.
- Data Recording and Review: Helps patients and healthcare providers identify hypoglycemia patterns and adjust treatment plans.






